What is Kyphoplasty?
Kyphoplasty is a minimally invasive procedure performed by Interventional Radiologists for the treatment of compression fractures causing back pain. The procedure aims to carefully inject cement into a compression fracture of vertebral body in the spine, thus reversing the instability, alleviating the back pain, correcting angular vertebral deformity, and restoring vertebral body height.
Who is a Candidate for Kyphoplasty?
Kyphoplasty may be an option for you if you are experiencing back pain specifically due to a compression fracture from one of the following diagnoses:
- osteoporosis
- metastatic tumor
- multiple myeloma
- vertebral hemangioma
Kyphoplasty cannot improve old and chronic spine fractures, and it will not reduce back pain caused by other reasons (such as herniated disc, compressed nerve roots, muscular issues, etc).
How is the balloon kyphoplasty performed?
Balloon kyphoplasty is performed by an interventional radiologist, who is a physician with expertise in minimally invasive procedures using imaging guidance. It is performed in an Angiography Suite that looks like an operating room, but has a small x-ray camera over it, which provides real-time imaging for the procedure.
Treatment for each vertebral compression fracture level typically takes less than one hour. Multiple fractures can be treated simultaneously, usually up to 3 levels in one procedure, except in special circumstances. It can be performed on an inpatient or outpatient basis and is usually performed with monitored anesthesia care (MAC). It rarely requires general anesthesia. Your physician will discuss which options are appropriate for you.
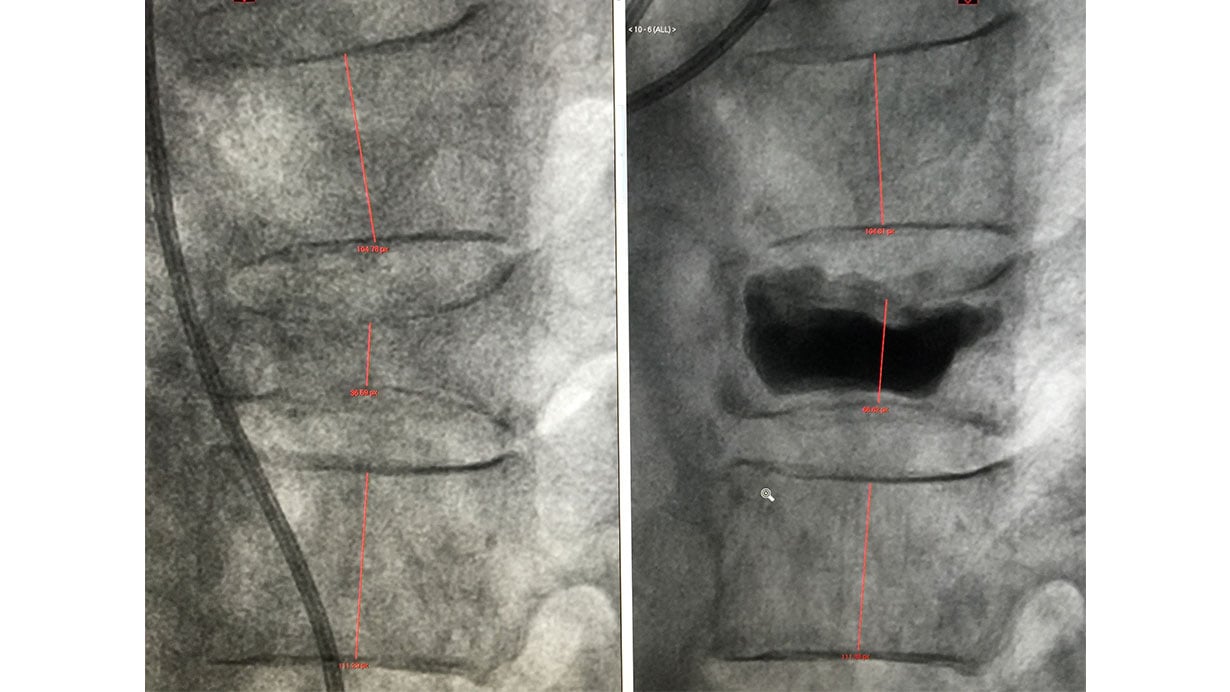
The procedure involves placing a metal cannula (about the size and diameter of a pencil) into the vertebral body to be treated using careful image guidance. Once the cannula is placed, a small balloon is advanced and carefully inflated under visualization, creating a cavity in the bone and condensing the bone around it, while trying to restore height to the vertebral body (called reducing the fracture).
Finally, a special sterile ‘bone cement’ called polymethylmethacrylate (PMMA) is injected into the bone. Injecting the bone cement has three purposes:
- As it hardens, it fixates the fractured portions of the bone (fractured bone movement is what causes the pain).
- It solidifies the structural rigidity of this portion of the spine that was acting as the “weak link in the chain.”
- The heat given off as the cement hardens has been hypothesized to burn tiny little nerve endings, which in turn reduces the pain.
How long will it take me to recover?
Balloon kyphoplasty is generally performed as an outpatient procedure. Following the procedure, you are transferred to the Interventional Radiology recovery area typically for a few hours for observation. After your sedation completely wears off, (usually within two hours) you will be asked to attempt walking if your pain has already subjectively improved. Your interventional radiologist will have a specific post-operative recovery/exercise plan to help you return to your normal daily life as quickly as possible.
Patients usually report relief from pain and are able to walk and move about soon after the procedure. Your doctor will schedule a follow-up visit and explain limitations, if any, on your activity.
How does balloon kyphoplasty differ from vertebroplasty?
Balloon kyphoplasty is similar to vertebroplasty; however, vertebroplasty does not include balloon inflation as a way to create a cavity prior to injection of the bone cement. Instead, the bone cement is directly injected into the bone after the cannula is placed. As no cavity is created, the bone cement injected needs to be thinner and under pressure, which equates to more risk for cement to leak out of the bone. In addition, no balloon inflation reduces the chance of restoration of height of the vertebral body.
What are the potential risks or complications of this procedure?
Kyphoplasty is a very safe procedure. At Rochester Regional Health, we have performed thousands of kyphoplasties over the past decade. Although the complication rate for balloon kyphoplasty is very low, as with most other surgical and minimally invasive procedures, serious adverse events can occur, some of which can be fatal. The following are the minor and major serious risks.
Minor risks and complications are more common than severe and may include - but are not limited to - bleeding/small hematoma on back, minor skin infection at site of injection, leakage of a small amount of “cement” into the adjacent disc space, and lack of pain relief despite successful technique during the procedure.
In more rare instances, major risks and complications may occur. These include cement embolism (leakage of the cement out of the vertebral body and migration to the lungs), paralysis (due to spinal cord damage), leakage of bone cement into the spinal canal and/or surrounding nerves (may also result in paralysis), severe infection of the vertebral body, disc space or spinal canal, and bleeding/hematoma in or surrounding the spinal canal, thus compromising the spinal cord.
